Heart Rhythm Disorders
Learn more about different heart rhythm disorders.


Heart Rhythm Disorders
Learn more about different heart rhythm disorders (also called arrhythmias) and how they can be diagnosed and treated by the cardiac electrophysiologists here at Parkwest Medical Center.
Looking for a Cardiologist at Parkwest Medical Center
For a physician referral, call 865-374-PARK (7275). You can also learn more about Parkwest cardiac services.
Types of Heart Rhythm Disorders
If you suffer from a heart rhythm disorder, you may suffer from some of the common examples below.
Atrial Fibrillation: This is an irregular, fast heart rhythm in the two upper chambers of your heart.
Bradycardia: This disorder causes your heartbeat to be too slow.
Tachycardia: With tachycardia, your heartbeat is too fast.
Ventricular Tachycardia: This is an extremely fast heartbeat.
Supraventricular Tachycardia: With this condition, you experience a sudden, very fast heartbeat.
Ventricular Fibrillation: Ventricular fibrillation is a fluttering of your heart muscle that doesn’t let it pump blood.
Sudden Cardiac Arrest: This occurs when your heart suddenly stops beating.
Long QT Syndrome: Long QT Syndrome can cause sudden abnormal rhythms of your heart.
Wolff-Parkinson-White (WPW) Syndrome: WPW Syndrome is a condition that causes you to have episodes of a fast heartbeat caused by an extra electrical pathway in the heart.
Other Arrhythmias: Other abnormal rhythms (arrhythmias) can be caused by pregnancy, medicine interactions, or metabolic problems.
Testing for Heart Rhythm Defects
Treatment for Heart Rhythm Disorders
Using cutting-edge, results-driven treatment, the high-performance heart team at Parkwest Medical Center can effectively manage your arrhythmia. We have a variety of available treatments to fit your needs and help you take care of your heart.


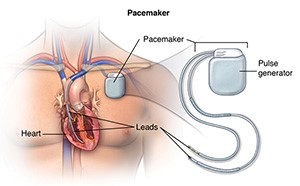 A pacemaker is a small device that is implanted under your skin (most often in the shoulder area just under the collarbone) that sends electrical signals to start or regulate a slow heartbeat.
A pacemaker is a small device that is implanted under your skin (most often in the shoulder area just under the collarbone) that sends electrical signals to start or regulate a slow heartbeat.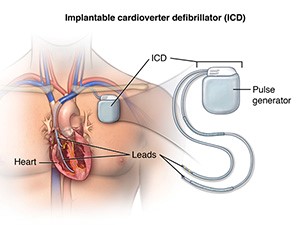 An implantable cardioverter defibrillator (ICD) looks very similar to a pacemaker, except that it is slightly larger. It has a generator, one or more leads, and an electrode for each lead.
An implantable cardioverter defibrillator (ICD) looks very similar to a pacemaker, except that it is slightly larger. It has a generator, one or more leads, and an electrode for each lead.